Sentinel trial
Skin patch trial could transform lung transplant care
Published on: 9 April 2026
Researchers at Newcastle University are at the forefront of a national trial exploring whether small patches of donor skin can act as an early, visible biomarker of lung transplant rejection,
The SENTINEL trial is testing whether donor skin grafts, transplanted alongside the same organ donor lungs, can signal immune rejection earlier, allowing faster intervention and potentially improving long‑term transplant outcomes.
Lung transplantation remains one of the most challenging solid organ transplants, with rejection rates of up to 30% in the first three to six months post‑transplant and five‑year survival of only around 50%.
Detecting rejection is particularly difficult, relying on frequent hospital attendance and invasive investigations such as bronchoscopy, transbronchial lung biopsies, imaging and blood tests.
Skin a visible immune sensor
The SENTINEL approach is based on the well‑established observation that skin allografts tend to reject earlier and more visibly than deeper organs.
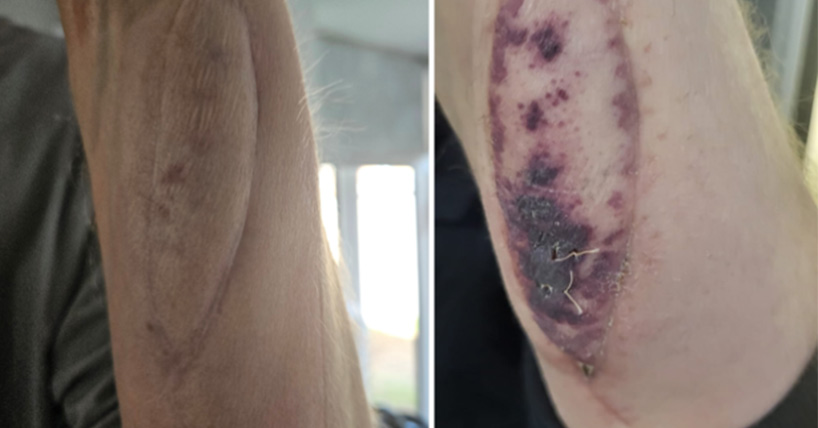
In the trial, patients receive a 10 cm × 3 cm patch of skin from the same organ donor, transplanted onto the forearm at the time of lung transplantation.
Researchers believe that immune rejection may first manifest as visible changes, such as erythema or rash, in the donated skin.
This allows clinicians to investigate rejection earlier, using a minimally invasive skin biopsy rather than a lung biopsy, and initiate treatment before irreversible damage occurs in the transplanted lung.
Andrew Fisher, Professor of Respiratory Transplant Medicine at Newcastle University and Honorary Consultant at Newcastle Hospitals, and Newcastle lead for the SENTINEL trial, said: “Early detection of rejection remains one of the most significant unmet needs in lung transplantation.
“This study is testing a biologically plausible and clinically elegant solution, using skin as a visible, accessible window into the immune response against a transplanted organ.
“If sentinel skin grafts reliably signal rejection earlier than current approaches, this could markedly reduce reliance on invasive lung biopsies and allow more timely, targeted immunosuppression.”
In addition to acting as an early warning system, the skin patch may also modulate immune responses to the lung graft itself, potentially reducing rejection rates overall.
Newcastle’s Freeman Hospital is one of five UK specialist cardiothoracic centres delivering the trial, with Newcastle University researchers contributing clinical expertise in respiratory and transplant medicine.

Patient supports trial
One of the first patients in the UK to receive a sentinel skin graft was treated in Newcastle.
Former bus driver Darren White, 52, from Stockton-on-Tees, underwent a lung transplant at Newcastle’s Freeman Hospital in late 2024 after being diagnosed with lung fibrosis earlier that year.
While on the transplant waiting list, Darren agreed to take part in the SENTINEL trial, receiving a small donor skin patch on his forearm alongside his lung transplant.
Three months after surgery, Darren noticed a rash on the donor skin patch. Although he felt well, he alerted his transplant team.
A biopsy confirmed very mild rejection, which was treated promptly with steroids, before his lungs were affected.
Darren said: “I’m a year post-transplant now and doing really well. Who knows if that would be the case if the rash hadn’t shown up and rejection wasn’t spotted until much further down the line.
“The trial is a truly fantastic thing, and I hope it goes on to show that a skin patch is a viable option for identifying rejection as early as possible.
“I’m eternally grateful to the trial team but most of all, to my donor’s family who made the selfless and incredibly generous decision to allow donation to go ahead, but to also agree to this extra donation, of the skin patch.”
While individual cases cannot determine trial outcomes, researchers say the experience illustrates the feasibility of patient‑led monitoring and reinforces the scientific rationale for the study.
Press release adapted with thanks to NHS Blood and Transplant.



