Transplant documentary
Experts feature in documentary showing pioneering transplant surgery
Published on: 11 May 2018
Some 50 years since the world’s first heart transplant, a BBC documentary looks at a year in the lives of patients in need of a new heart, and the medics using cutting-edge technology to treat them.
World-experts at Newcastle University are filmed at the Freeman Hospital’s Institute of Transplantation, where the programme follows seven patients as they wait for a donor heart to become available.
Aged from eight months to 56 years, their stories reveal the realities of the donation and transplant process. What life is like for those waiting for a donor heart to become available, how donor organs are found, and the extraordinary complexities of the surgery itself.
The programme also reveals a pioneering new technology which leading surgeons believe could improve the prognosis for the thousands of patients waiting for a transplant.
The programme 'Heart Transplant: A Chance to Live' is on BBC Two on Monday 14 May, 9pm and then available on the BBC iplayer.
Difficulties faced
John Dark, Professor of Cardiothoracic Surgery at Newcastle University, retired from clinical work last year, following 30 years as a leading heart and lung transplant surgeon at the Freeman Hospital.
He said: “This programme gets to the centre of the problems in heart transplantation. It shows the agonies of the wait for a new organ, and the difficult decisions for the surgeons.
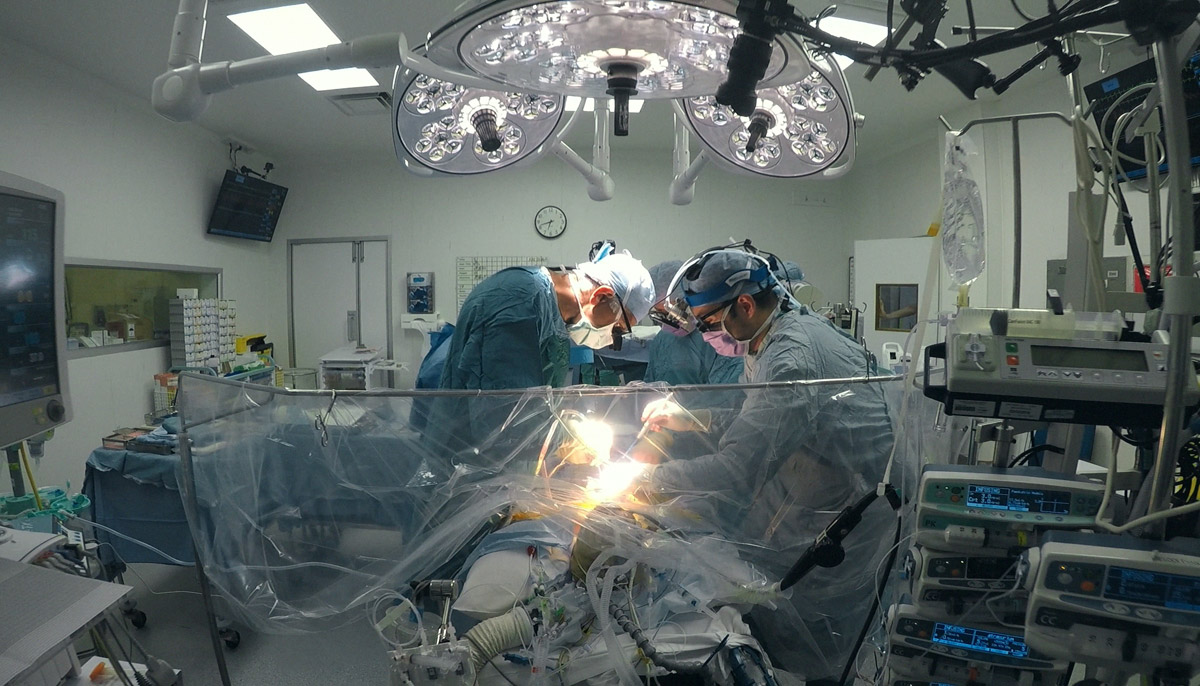
“The operating theatre scenes are an incredibly real portrayal of the difficulties we face and the way the team pulls together to overcome them.
“Organ perfusion is poised to make a big contribution to increasing the numbers of transplants we can do. The Organ Care system is just the first step in a rapidly evolving field.
“The research we are doing at Newcastle University and the Freeman Hospital is helping us bring the benefits of this technology to all organs, to benefit patients across the whole range of transplants.”
There is a shortage of suitable organs donated for transplant with the average adult waiting more than 1,200 days for a heart transplant.
Surgeons have been searching for an answer to this problem for years - and now believe they have made the pivotal breakthrough.

Pioneering surgery
Using an extraordinary process called Ex Vivo Perfusion, doctors can reanimate hearts, medicate them and keep them alive outside the body. This helps to keep the deterioration process at bay whilst they are transported to the recipient patient.
This means organs can be transported from much further away, widening the donor pool. It also gives doctors much more time to assess an organ’s function, reducing the risk of failure inside the recipient post-transplant.
Doctors believe that harnessed correctly, this technology could double the number of organ transplants performed in this country.
Asif Hasan, director of cardiopulmonary transplantation and cardiac surgeon, describes the new system as “a game changer in the way we prepare hearts for transplant.”
Mr Hasan said: “As soon as a heart is removed from the donor’s body it ceases to pump blood and oxygen into the muscle. The heart becomes oxygen starved and muscles cells begin to die.
“Traditionally we have transported donor hearts in ice to try to slow the deterioration rate and we have had a four hour window in which to get the heart from the donor to the hospital, where we have someone in need of a new heart waiting.
“During this time we need to assess its health and whether or not it is actually compatible for the recipient patient so we cannot start to prepare the patient for surgery until we know for sure.
“In all this time the heart’s function is diminishing and with it, the best chances of a successful transplant. So we are under a great deal of pressure to get surgery underway as soon as possible.”
With unprecedented access to the world class surgeons at the Freeman Hospital, this film will, for the first time, show this amazing new technology in action.
Heart Transplant: A Chance to Live" (BBC Two) Monday 14 May, 9pm.



